

Five care homes closed, 550 beds canceled. That was Hamburg in 2024 - not because of a lack of residents, not because of renovations. Because there was no staff.
What made the headlines in Hamburg has long since become part of everyday life in Mecklenburg-Western Pomerania, Saarland and parts of Bavaria. Outpatient services are rejecting clients. Wards are being merged. PDLs draw up duty rosters that are already a waste of time on the third day of the month because someone is ill again and the leasing agency can no longer send anything.
This article is aimed at management and HR managers who want to know where the journey is heading, which figures are reliable and, above all, what they can do concretely before the scope becomes even narrower.

What exactly does „care crisis“ mean?
A nursing crisis is a situation in which there are not enough qualified nursing staff available to cover the care requirements in hospitals, nursing homes and outpatient services. Germany has been experiencing this situation for over a decade. But what we are experiencing today has little in common with the bottlenecks of 2015. It is no longer a bottleneck. It is a structural deficit that is deepening with each passing year.
Current figures: How big is the supply gap really?
At the end of 2023, there were 5.7 million people in need of care in Germany. 86% of them are cared for at home, mainly by relatives. The care insurance statistics make the dynamic visible: in 2017, there were still 3.3 million. In eight years, the number has almost doubled. By 2055, the Federal Statistical Office expects the number to reach 6.8 million.
On the supply side, the Federal Statistical Office published its nursing staff forecast in January 2024. The key finding: demand will increase from 1.62 million nurses (base year 2019) to 2.15 million in 2049, i.e. by a third. In the most favorable scenario, there will be a shortage of 280,000 skilled workers by then. In the least favorable scenario, which only takes into account demographic developments without positive labor market trends, the shortfall is 690,000.
By 2034, the gap will be at least 90,000. Outpatient care is particularly affected, with an additional demand of 60 percent. In inpatient care for the elderly, the figure is 39% and in hospitals 14%.
And there is one figure that is missing from most industry reports: the labor market reserve. It describes how many job-seeking nurses are theoretically available. In 2025, it was 2.0 percent. By 2027, it will have halved to 1.0 percent. In plain language, this means that there is almost no one left who can be reached via job advertisements.
Regional differences: For some regions, it is already too late for half measures
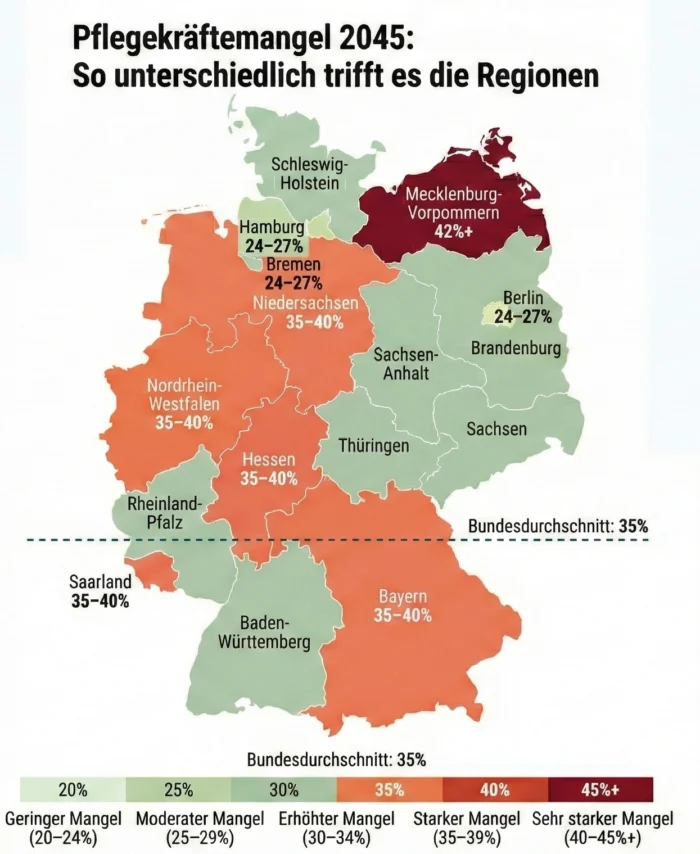
Germany is talking about the shortage of nursing staff as if it were affecting the country equally. This is not true. Greifswald and Munich, Saarland and Berlin are worlds apart.
In April 2025, Prognos AG calculated the percentage of demand for elderly care that cannot be met in the individual regions by 2045. The national average is 35 percent. Mecklenburg-Western Pomerania is the worst off with over 42 percent. In Bavaria, the forecast is negative in 14 of the 20 districts surveyed. Saarland, large parts of North Rhine-Westphalia, Hesse and Lower Saxony are also above average.
Things look better in the city states: Berlin comes in at 24%, Hamburg at 25% and Bremen at 27%, not because they are better at recruiting staff, but because large cities have a younger population structure. However, 24 percent unmet demand is still a situation in which every fourth request comes to nothing.
What does this mean for employers? A nursing home in Rostock needs a fundamentally different HR strategy than a provider in Cologne. If you are located in a region with a 40+ percent forecast and rely exclusively on the local labor market, you are planning your own closure.
Why it has come to this
Much is written about the causes of the shortage of nursing staff, often in a way that suggests that a single adjusting screw can be turned. This is nonsense. There are five mutually reinforcing factors that cannot be broken without simultaneous countermeasures.
Demographics: more patients and fewer staff at the same time
Baby boomers are in need of care. That alone would be a challenge. At the same time, however, the baby boomers among the nursing staff are also retiring. According to the Curacon sector report Altenhilfe 2024, 43% of geriatric nurses across Germany are over 50 years old. They will retire in the next ten to fifteen years.
Moving up does too little. Nothing pushes from below. The age pyramid is tilting on both sides of the care bed at the same time.
Working conditions that drive people away
Nobody becomes a care worker because they find the salary attractive. People go into nursing because they want to help. And they leave because the system makes it impossible for them to help.
72 percent of nursing staff in management positions cite physical stress as a serious problem (PwC 2022). 59 percent cite mental stress. What statistics do not record: anger about the tenth changed duty roster in a row, the feeling of not having provided good enough care in the evening because three colleagues were absent. 63 percent of young people between 18 and 29, who could imagine working in nursing in principle, fear precisely this psychological strain. Before they have even started.
40 percent of active nursing staff regularly think about quitting. This is not a survey from 2015, this is the current situation.
A profession that more people leave than enter
Together with the RWI-Leibniz Institute, the Bertelsmann Stiftung published an analysis in 2025 that gets to the heart of the problem: from 2022 to 2023, 191,000 people left so-called bottleneck occupations. Only 167,000 came in the opposite direction. That's a net loss of 24,000 skilled workers in one year.
In the care sector, the findings are even more bitter: two thirds of those who leave the health and care sector change careers completely. Administration, retail, logistics. What they have taken with them, namely ten or fifteen years of experience in dealing with the seriously ill, cannot be retrained in six months.
Part-time as a survival strategy
Every second nurse works part-time. In no other sector with a comparable shortage of skilled workers is the proportion so high. The usual explanation points to the 82 percent share of women. But this does not go far enough: the proportion of part-time work among male care workers is also almost a third. For all men in Germany who are subject to social insurance contributions, the figure is 13 percent.
Part-time work in care is often not an expression of a life plan. It is a protective reflex. Anyone who works 40 hours under these conditions will burn out after five years. If you cut back to 25 hours, you might be able to do the job for another ten years. From an employer's perspective, this means that every hour that a skilled worker would work more if the conditions were right is an hour that does not need to be recruited.
Training: many beginners, too few degrees
In 2023, 53,900 new training contracts for nurses were concluded nationwide, three percent more than in the previous year. Sounds like a trend reversal. But it's not.
At the same time, over 41% of the first graduating class of 2023 in NRW completed their training without taking an exam (IT.NRW). In Berlin and Brandenburg, the dropout rates were around 42%. Nationwide, estimates vary between 25 and 37 percent, depending on the methodology used. In a panel survey, the BIBB (Federal Institute for Vocational Education and Training) found that almost half of the trainees surveyed thought about dropping out at least occasionally.
The causes are an open secret. Trainees are scheduled as fully-fledged staff on the ward from the tenth week onwards, because otherwise the duty roster doesn't work out. Practice supervisors who have no time for guidance themselves. An everyday working life that corresponds exactly to what the campaigns actually wanted to portray in a more positive light.
The only encouraging aspect is that over 30 percent of people who started nursing training in 2023 were older than 30. The profession therefore also works as a second or third career. But career changers need entry models that suit their lives: Part-time training, adapted practical assignments, financial bridges.
Effects on facilities and providers
The facts speak for themselves here too. The Federal Employment Agency puts the average vacancy period for nursing staff at 160 days. The average for all professions is 120. In rural geriatric care, a position can easily remain vacant for nine months or longer.
For a PDL, this means constantly juggling with leased staff who are more expensive, don't know the building and leave after three weeks. Overtime accounts that are regularly in the red. A team that wonders why they are working so hard while temporary workers are standing next to them for significantly more money.
The new staffing assessment procedure in inpatient geriatric care further exacerbates the situation. It prescribes more precise staffing ratios. The transition period expired at the end of 2025. Facilities that do not provide evidence of the required staffing ratio risk regulatory measures. In theory, a useful instrument for quality assurance. In practice, an accelerator of the shortage: demand increases, supply remains the same.
At system level, the next crisis is just around the corner anyway. In 2025, the Federal Audit Office warned of a funding gap of up to 12.3 billion euros in long-term care insurance by 2029.
Strategies that work: What employers can do
There is no single solution to the shortage of skilled nursing staff. But there are measures whose impact has been proven by figures. The facilities that will still be able to act in five years' time are those that operate several levers simultaneously today.
International nursing staff: the only factor that has been growing since 2022
That is the one sentence employers should take away from this article: Since 2022, employment growth in the German care sector has been driven exclusively by foreign skilled workers. The number of nursing staff with a German passport is falling. In geriatric care, it fell by four percent in 2023/2024. Anyone who thinks this is a side note has not understood the situation.
Over 300,000 foreign nursing staff were working in Germany in 2024, 17.8 percent of all nursing staff. In 2013, there were 75,000. 27,000 were added between June 2023 and June 2024 alone. Almost one in four care workers in retirement homes is now of a different nationality (IAB Research Report 22/2024, Federal Employment Agency, Integration Media Service).
Without international recruitment, German nursing would have been on the decline for three years. This is not an opinion piece. These are the official labor market data.
International recruitment: a comparison of four paths
Recruitment channels at a glance
Employers who want to recruit international staff now have several options. The right approach depends on the size of the organization, the budget and the desired speed.
The Triple Win Program of the Federal Employment Agency places nursing staff from Bosnia-Herzegovina, the Philippines, Tunisia, Indonesia, India and Jordan. Language preparation and recognition support are part of the package. The disadvantage: limited capacity and long lead times. Often too slow for institutions that need staff within six months.
The Western Balkans regulation, introduced in 2015 and now time-limited, has increased the number of care workers from the Western Balkans fivefold to over 51,000. Bureaucratic hurdles are relatively low. However, there is no language preparation and quality assurance is entirely the responsibility of the employer.
The Skilled Immigration Act, amended in 2023, has been expanded with the opportunity map, the recognition partnership and the Accelerated skilled worker procedures significantly expanded the legal framework. 13,000 care workers came via this route in 2024. Visas issued in around four months.
Specialized placement agencies like TalentOrbit take over the process from candidate selection to language courses and integration on site. This is more expensive than the state programs, typically 15,000 to 30,000 euros per skilled worker. In return, the speed is faster, the support is more individual and, based on the experience of recent years, the likelihood of staying is significantly better. Anyone who only fills positions without investing in integration is saving money at the wrong end.
Within the EU, most nursing staff come from Poland, Croatia and Romania. However, the trend is downwards, as these countries are also experiencing their own shortage of skilled workers. The growth area is third countries: Turkey, Serbia, Bosnia-Herzegovina, the Philippines, India, Tunisia and Vietnam. Also Georgia is gaining in importance: a country with a solid tradition of medical training and specialists who want to stay for the long term. A comprehensive guide to the entire process can be found in the article Hiring nursing staff from abroad.
Where practice gets stuck. The recognition of foreign professional qualifications is an imposition in some federal states. Those affected report waiting times of up to four years. The result: motivated, well-trained specialists who remain formally classified as nursing assistants. Hiring international nursing staff without planning for the recognition period is a recipe for frustration on both sides. Realistic time planning and cooperation with experienced intermediaries is not an additional service, but a basic requirement.
Retaining existing staff: cheaper than any new recruitment, but still neglected
It is a paradox that is constantly observed in the industry: Institutions spend five-figure sums on recruiting and leasing, while their own people work in conditions that could be improved with a fraction of the money.
In almost every survey, reliable duty scheduling is the number one wish of employees. Even before salary. If you can assure your employees that the schedule is fixed and will not be changed over the phone at the weekend, you will measurably increase their willingness to work full-time. It is the cheapest lever against staff shortages, and it is surprisingly rarely used consistently.
Something has changed in terms of salary. Trained nursing staff now earn above the average for all training occupations: 4,067 euros in the nursing sector, 3,920 euros in geriatric nursing (Destatis 2023). That is more than many people expect. The problem is that the workload is also far above average. Money alone doesn't keep anyone. Money plus reliable working hours plus company health management? That's a different calculation.
Winning back former nursing staff
Every second person who has left nursing care can imagine returning to it. Every second person! That's a potential that most facilities don't even begin to tap into.
What these people don't need is an Instagram post with the hashtag „PflegeIstHerzensarbeit“. What they need is a phone call from someone who knows them and an honest offer: ten hours a week to get started, a permanent contact person, a realistic picture of what has and hasn't changed in the home. Some institutions have launched targeted return programs in the last two years. The initial experiences are promising.
Digitalization: not a miracle cure, but an underestimated lever
Technology does not replace a caregiver. Period. Anyone who says that has never worked in nursing. What technology can do is reduce the bureaucratic ballast that eats up up to half of nursing staff's working time.
In practice, voice-controlled documentation saves up to 30 minutes per shift. Extrapolated to an entire team and a whole year, that's hundreds of hours of skilled labor. Fall sensors and vital signs monitoring take the strain off night shifts. Transport robots take over physically demanding routines.
However, only a fraction of the available federal funding for care digitization has been used so far. Many facilities not only lack the budget, but above all someone to manage the introduction. Those who take the lead here will become more attractive employers for younger professionals. Those who wait until everyone else is ready will have lost staff in the meantime.
Outlook: What happens if nothing changes
Without other strategies, it will not be possible to meet a third of the demand for elderly care throughout Germany by 2045. In some regions, almost half.
The international environment is exacerbating the situation: 15 EU countries are reporting similar nursing staff shortages (OECD, Health at a Glance 2024). Scandinavia, the Gulf States, Canada and the United Kingdom are competing for the same skilled workers. Germany has followed suit with its Skilled Immigration Act, but other countries offer faster recognition procedures and in some cases higher salaries. If you want to attract international nursing staff, you don't just have to compete with your neighbor around the corner, but also with London and Dubai.
At the same time, the figures show that targeted measures are working. From 75,000 to over 300,000 international nursing staff in a decade: this is no coincidence, but the result of political framework conditions and entrepreneurial decisions.
Conclusion
In no other sector are rhetoric and action as far apart as in the care sector. Everyone is talking about the emergency. Very few are taking action.
The conclusion that follows from the labor market data of the last three years is uncomfortable, but clear: domestic measures alone are not enough in terms of figures. Training does not even compensate for retirement, let alone growth in demand. Recruiting former skilled workers is an important lever, but limited in scope. Digitalization eases the burden, but does not create new minds. Without international recruitment, the care sector will shrink.
This does not mean that the other strategies are unimportant. It means that employers who want to remain capable of acting must invest at all levels at the same time: attract internationally, retain internally, reduce the digital burden, improve training. If you operate a single lever and wait for the rest, you will close stations.
→ How TalentOrbit supports employers in international recruitment
Frequently asked questions
Sources:
Federal Statistical Office (Destatis): Pflegekräftevorausberechnung 2019-2049, January 2024 - Federal Statistical Office (Destatis): Pflegestatistik 2023 - Federal Employment Agency: Arbeitsmarktsituation im Pflegebereich, Berichte Blickpunkt Arbeitsmarkt, 2025 - IAB-Forschungsbericht 22/2024: Ausländische Beschäftigte in den Pflegeberufen - Mediendienst Integration: Factsheet Ausländische Pflegekräfte und Ärzte, May 2025 - Bertelsmann Stiftung / RWI-Leibniz-Institut für Wirtschaftsforschung: Fachkräftemangel und Berufswechsel, 2025 - Prognos AG: Pflege 2045 - Regionale Fachkräfteprognose, April 2025 - PwC: Fachkräftemangel im deutschen Gesundheitswesen, 2022 - Curacon: Branchenreport Altenhilfe, 2024 - IT.NRW: Nursing training statistics, press release May 2024 - Office for Statistics Berlin-Brandenburg: Nursing training statistics 2023 - BIBB: Research project on training dropouts in nursing - German Nursing Council: Factsheet DPT25 - OECD: Health at a Glance, 2024
Last updated: February 2026

